Scientists develop a low-cost device to make cell therapy safer
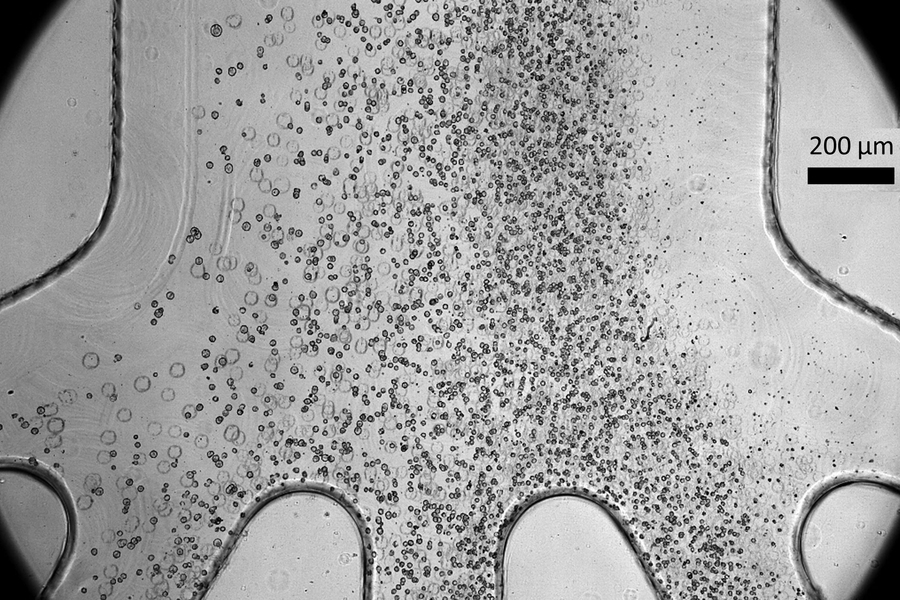 Scientists developed a tiny microfluidic device that can improve the safety and efficacy of cell therapy techniques for spinal cord injury patients. Their device, which can sort cells by size as shown in the photo, can remove a large percentage of stem cells that have not yet fully become spinal cord cells, which could potentially form tumors after being transplanted into a patient.
Image courtesy of the researchers.
Scientists developed a tiny microfluidic device that can improve the safety and efficacy of cell therapy techniques for spinal cord injury patients. Their device, which can sort cells by size as shown in the photo, can remove a large percentage of stem cells that have not yet fully become spinal cord cells, which could potentially form tumors after being transplanted into a patient.
Image courtesy of the researchers. A tiny device built by scientists at MIT and the Singapore-MIT Alliance for Research and Technology could be used to improve the safety and effectiveness of cell therapy treatments for patients suffering from spinal cord injuries.
In cell therapy, clinicians create what are known as induced pluripotent stem cells by reprogramming some skin or blood cells taken from a patient. To treat a spinal cord injury, they would coax these pluripotent stem cells to become progenitor cells, which are destined to differentiate into spinal cord cells. These progenitors are then transplanted back into the patient.
These new cells can regenerate part of the injured spinal cord. However, pluripotent stem cells that don’t fully change into progenitors can form tumors.
This research team developed a microfluidic cell sorter that can remove about half of the undifferentiated cells — those that can potentially become tumors — in a batch, without causing any damage to the fully-formed progenitor cells.
The high-throughput device, which doesn’t require special chemicals, can sort more than 3 million cells per minute. In addition, the researchers have shown that chaining many devices together can sort more than 500 million cells per minute, making this a more viable method to someday improve the safety of cell therapy treatments.
Plus, the plastic chip that contains the microfluidic cell sorter can be mass-produced in a factory at very low cost, so the device would be easier to implement at scale.
“Even if you have a life-saving cell therapy that is doing wonders for patients, if you cannot manufacture it cost-effectively, reliably, and safely, then its impact might be limited. Our team is passionate about that problem — we want to make these therapies more reliable and easily accessible,” says Jongyoon Han, an MIT professor of electrical engineering and computer science and of biological engineering, a member of the Research Laboratory of Electronics (RLE), and co-lead principal investigator of the CAMP (Critical Analytics for Manufacturing Personalized Medicine) research group at the Singapore-MIT Alliance for Research and Technology (SMART).
Han is joined on the paper by co-senior author Sing Yian Chew, professor of chemistry, chemical engineering, and biotechnology at the Lee Kong Chian School of Medicine and Materials Science and Engineering at Nanyang Technological University in Singapore and a CAMP principal investigator; co-lead authors Tan Dai Nguyen, a CAMP researcher; Wai Hon Chooi, a senior research fellow at the Singapore Agency for Science, Technology, and Research (A*STAR); and Hyungkook Jeon, an MIT postdoc; as well as others at NTU and A*STAR. The research appears today in Stem Cells Translational Medicine.
Reducing risk
The cancer risk posed by undifferentiated induced pluripotent stem cells remains one of the most pressing challenges in this type of cell therapy.
“Even if you have a very small population of cells that are not fully differentiated, they could still turn into cancer-like cells,” Han adds.
Clinicians and researchers often seek to identify and remove these cells by looking for certain markers on their surfaces, but so far researchers have not been able to find a marker that is specific to these undifferentiated cells. Other methods use chemicals to selectively destroy these cells, yet the chemical treatment techniques may be harmful to the differentiated cells.
The high-throughput microfluidic sorter, which can sort cells based on size, had been previously developed by the CAMP team after more than a decade of work. It has been previously used for sorting immune cells and mesenchymal stromal cells (another type of stem cell), and now the team is expanding its use to other stem cell types, such as induced pluripotent stem cells, Han says.
“We are interested in regenerative strategies to enhance tissue repair after spinal cord injuries, as these conditions lead to devasting functional impairment. Unfortunately, there is currently no effective regenerative treatment approach for spinal cord injuries,” Chew says. “Spinal cord progenitor cells derived from pluripotent stem cells hold great promise, since they can generate all cell types found within the spinal cord to restore tissue structure and function. To be able to effectively utilize these cells, the first step would be to ensure their safety, which is the aim of our work.”
The team discovered that pluripotent stem cells tend to be larger than the progenitors derived from them. It is hypothesized that before a pluripotent stem cell differentiates, its nucleus contains a large number of genes that haven’t been turned off, or suppressed. As it differentiates for a specific function, the cell suppresses many genes it will no longer need, significantly shrinking the nucleus.
The microfluidic device leverages this size difference to sort the cells.
Spiral sorting
Microfluidic channels in the quarter-sized plastic chip form an inlet, a spiral, and four outlets that output cells of different sizes. As the cells are forced through the spiral at very high speeds, various forces, including centrifugal forces, act on the cells. These forces counteract to focus the cells in a certain location in the fluid stream. This focusing point will be dependent on the size of the cells, effectively sorting them through separate outlets.
The researchers found they could improve the sorter’s operation by running it twice, first at a lower speed so larger cells stick to the walls and smaller cells are sorted out, then at a higher speed to sort out larger cells.
In a sense, the device operates like a centrifuge, but the microfluidic sorter does not require human intervention to pick out sorted cells, Han adds.
The researchers showed that their device could remove about 50 percent of the larger cells with one pass. They conducted experiments to confirm that the larger cells they removed were, in fact, associated with higher tumor risk.
“While we can’t remove 100 percent of these cells, we still believe this is going to reduce the risk significantly. Hopefully, the original cell type is good enough that we don’t have too many undifferentiated cells. Then this process could make these cells even safer,” he says.
Importantly, the low-cost microfluidic sorter, which can be produced at scale with standard manufacturing techniques, does not use any type of filtration. Filters can become clogged or break down, so a filter-free device can be used for a much longer time.
Now that they have shown success at a small scale, the researchers are embarking on larger studies and animal models to see if the purified cells function better in vivo.
Nondifferentiated cells can become tumors, but they can have other random effects in the body, so removing more of these cells could boost the efficacy of cell therapies, as well as improve safety.
“If we can convincingly demonstrate these benefits in vivo, the future might hold even more exciting applications for this technique,” Han says.
This research is supported, in part, by the National Research Foundation of Singapore and the Singapore-MIT Alliance for Research and Technology.
Media Inquiries
Journalists seeking information about EECS, or interviews with EECS faculty members, should email eecs-communications@mit.edu.
Please note: The EECS Communications Office only handles media inquiries related to MIT’s Department of Electrical Engineering & Computer Science. Please visit other school, department, laboratory, or center websites to locate their dedicated media-relations teams.